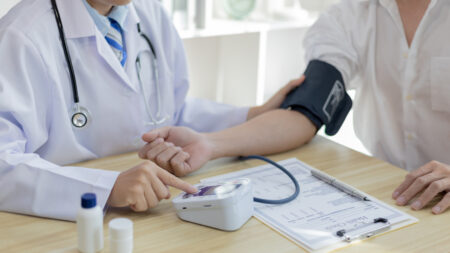
The study has shown role of Vitamin D in development of dopaminergic neurons and how it may cause disorders like schizophrenia.
According to a study published in the Journal of Neurochemistry, the researchers have confirmed the critical significance of maternal vitamin D levels in the development of the brain cells that produce dopamine the ‘feel-good’ hormone of the body, with the help of molecular imaging technology. The discovery provides a closer look into the mechanisms underlying neurodevelopmental disorders such as schizophrenia.
Schizophrenia is a chronic brain disorder with symptoms including hallucinations, difficulty thinking, delusions, disorganized speech, and lack of motivation among others.
It is believed that a combination of genetic and environmental factors contribute to the development of schizophrenia. The exact method by which it does this is uncertain, but there is compelling evidence that the disorder alters the brain’s ability of using dopamine.
The Hypothesis
Exposure to schizophrenia risk factors during embryonic development is believed to change the way dopamine circuits are formed in the brain. Past research work has found low maternal vitamin D levels to be one such risk factor, exerting an influence on the differentiation of dopamine-producing (dopaminergic) neurons into their mature, specialized form.
A group of researchers from the University of Queensland’s Brain Institute have used molecular imaging techniques to expand on previous studies and thoroughly examine the relationship between vitamin D, dopaminergic neurons, and schizophrenia.
The Research
To mimic the differentiation process that takes place during an embryo’s development, the researchers created dopamine-like neurons. These neurons were then cultured both in the presence and absence of the hormone calcitriol. Vitamin D that has been ingested is not active until it has gone through two enzymatic processes in the body, the second of which takes place in the kidney where it is transformed into calcitriol, the active form of vitamin D. Calcitriol binds to the vitamin D receptors in the cell’s nucleus and activates them.
The scientist’s found that vitamin D did not only have an impact on cell differentiation but also on neuron’s structure.

Darry Eyles, the study’s corresponding author said that they discovered that the altered differentiation process in vitamin D’s presence not only caused cells to grow differently but also recruits machinery to release dopamine differently.
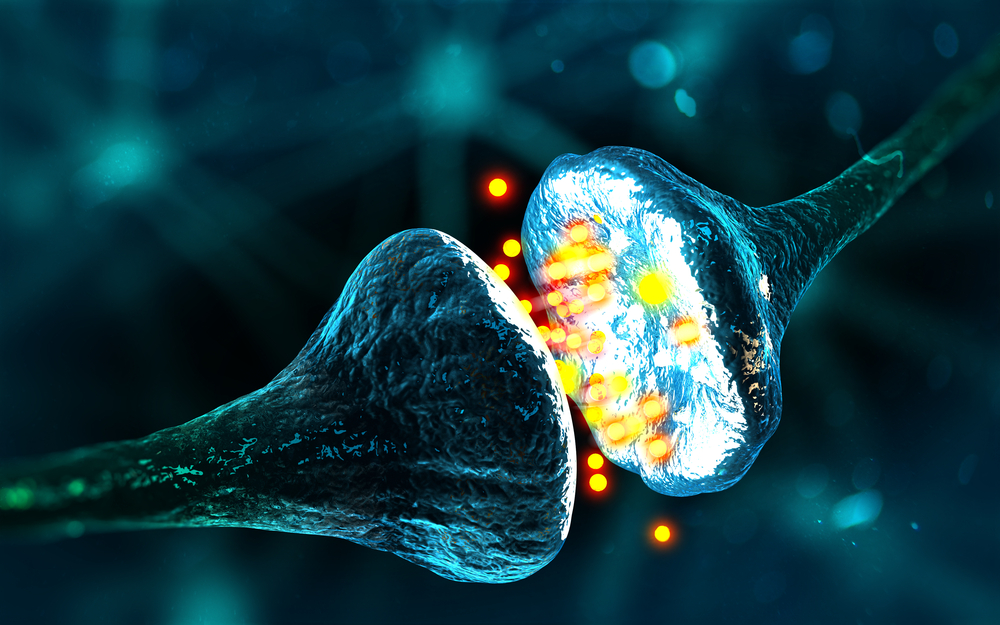
The machinery includes the neurites, which project from a neuro’s cell body. Neurites are essential to send signals to and from other parts of the nervous system. The scientists discovered the number of neurites was noticeably enhanced, and within those neurites, the proteins responsible for releasing dopamine showed altered localization.
The scientists were able to examine how dopamine uptake and release altered in the presence or absence of calcitriol using a brand-new imaging technique called False Fluorescent Neurotransmitters (FFNs). Small-molecule dyes called FFNs closely mimic the effects of neurotransmitters like dopamine. They make it possible to image both the storage and release of individual molecules at nerve terminals.
The Findings
They discovered that dopamine release was higher in neurons cultured in the presence of calcitriol when compared to a control.
According to Eyles, this is clear evidence that vitamin D impacts the structural differentiation of dopamine -producing neurons.

With the help of FFNs to target and observe single dopamine molecules the researchers have been able to confirm their long-held hypothesis that the levels of vitamin D during development impacted the formation of dopamine -producing neurons. They think that the dopamine dysfunction found in adult schizophrenia may be caused by early alterations in dopamine neuron development and function.
If other environmental risk factors for schizophrenia, such as low oxygen levels or infection during pregnancy, also affect how dopamine neurons develop, the researchers aim to look into that soon.