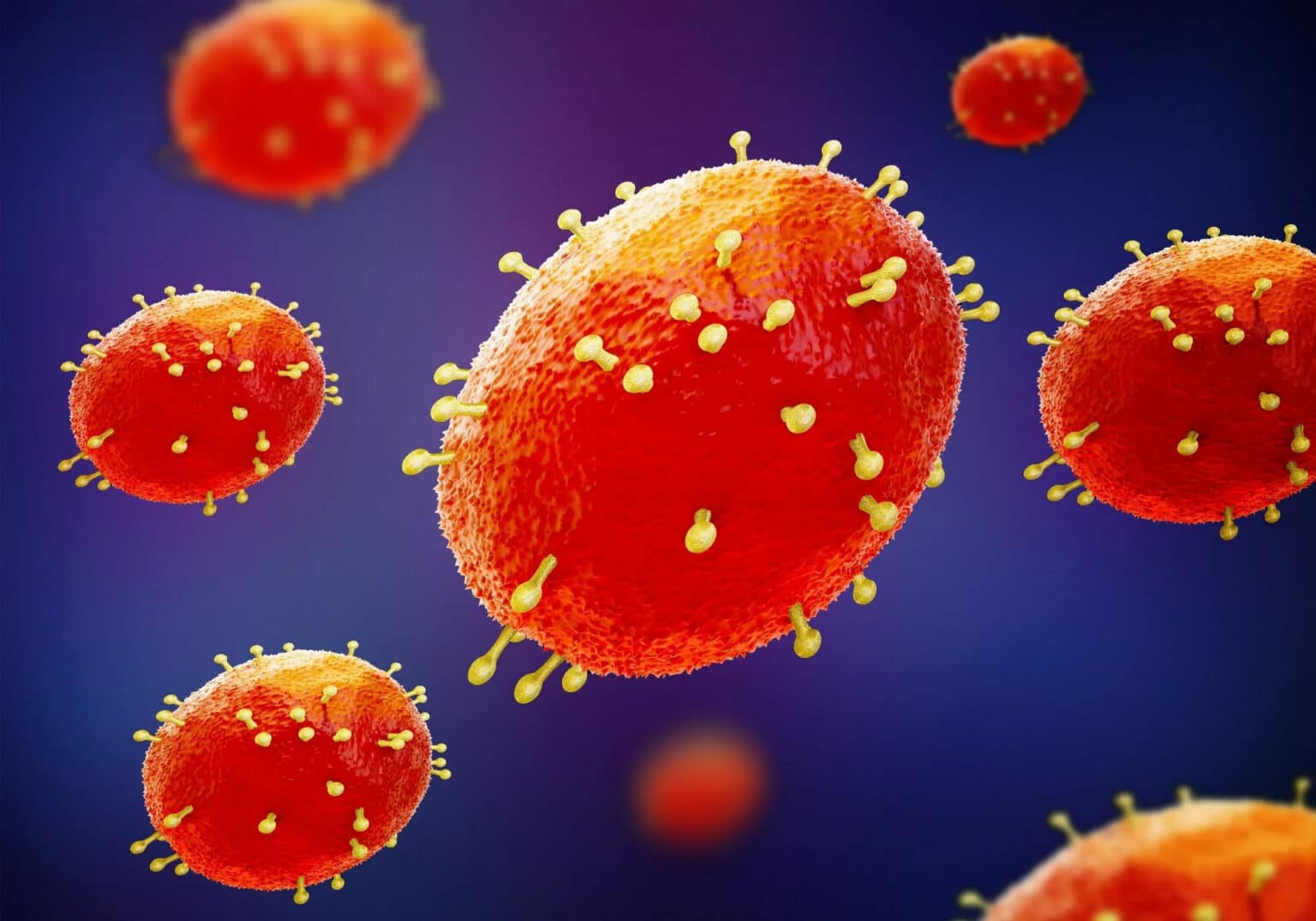
People living with HIV account for 40-50% of the people affected by Mpox. Emerging data and clinical shreds of evidence show higher fatality in people with more advanced HIV. The death rate among these patients is 15%.

Image credit: Gavi, the Vaccine Alliance
Table of Contents
What is Mpox?
Mpox, previously known as monkeypox, is a zoonotic viral disease, was first diagnosed in humans in 1970 in the Democratic Republic of Congo in Africa. It produces symptoms similar to smallpox but is less contagious and currently has a 3-6% of case fatality ratio. It spreads from one individual to the other by close contact with lesions, body fluids, and respiratory droplets of infected individuals as well as contaminated materials such as bedding. Mpox generally presents clinically with fever, rash, and swollen lymph nodes and may lead to a range of other medical complications.
Since the disease is caused by a virus similar to and from the same family as the smallpox virus, vaccines used to eradicate smallpox provides protection against mpox. An antiviral agent developed has been licensed for the treatment of mpox.
WHO on Mpox
WHO announced that it will prefer to call the disease ‘Mpox’ and phased out the name ‘monkeypox’ to lessen the irrelevant negative impact of names on trade, travel, tourism, or animal welfare, and abstain from causing offense to any cultural, and social, national, regional, professional or ethnic groups.
The Mpox outbreak began spreading around last May in the year of 2022. Despite the number of cases depreciating in most regions, it has so far affected roughly 86,000 people in 110 countries and killed 92. WHO confirmed in a statement that the USA has been the most affected followed by Brazil, France, Spain, Columbia, Mexico, Peru, the UK, Germany, and Canada.
According to the latest statement, WHO assessed the global risk as ‘Moderate’. Regionally, WHO assessed the risk in the Region of America as ‘High’ and as ‘Moderate’ in the African region, Eastern Mediterranean region, European region, and South-East Asia region. The risk in the Western Pacific Region is considered as ‘Low’.

Image Credit: CIDRAP
New Study
In the new study, Queen Bary University and Barts Health NHS Trust of London tracked 382 adults infected with mpox in 28 countries who had advanced H.I.V. disease. They analyzed the amount of H.I.V. and the count of CD4 cells, a marker of the immune system, in these patients. The normal range for CD4 cells is from 500 to 1,500 per cubic millimeter of blood. All 27 deaths in the study were among people who had less than 200 CD4 cells. This viral disease killed about 30% of those with fewer than 100 CD4 cells.
The nature of the illness varies differently in patients with weakened immune systems. Although most people infected with mpox show lesions only at the site of exposure, those with advanced H.I.V. developed large, ulcerated lesions with the virus disseminated throughout the body.
One of the doctors said as the immune system is not able to contain the virus at all, the virus is everywhere- on the back, feet, in the eyes. It was observed many patients also had nodules in the lung that caused acute respiratory distress. Patients would need to take antibiotics to prevent other opportunistic infections, and should be offered two doses of vaccine injected under the skin, instead of between the layers of the skin as is presently practiced.
Not everyone with HIV is at risk of catching this type of mpox but still, the researchers suggest testing for HIV when infected with it. It is prevalent among bisexual and gay men. Awareness should be spread among the masses to take two doses of the mpox vaccine especially in the areas of low-level diagnosis or without universal free access to antiretroviral treatment. Addition of the disease to the list of opportunistic infections in people with advanced H.I.V. would motivate healthcare givers to identify and prioritize the patients most at risk of severe disease and death.