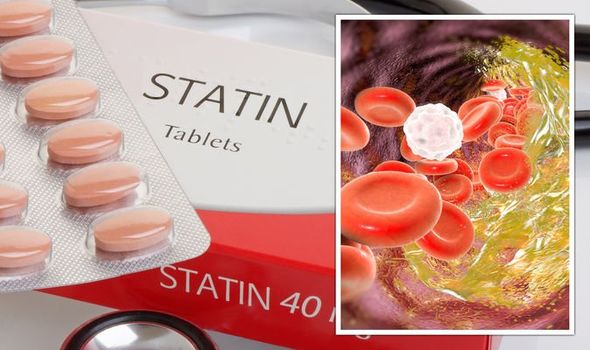
People who have had stenting or even a heart attack sometimes misbelieve that they no longer require medication to decrease their cholesterol. They believe that since their blockage has been treated surgically or medically, and they have been advised to modify their lifestyle while taking cardiac medications, the likelihood of their cholesterol levels increase is low. They frequently stop taking cholesterol-lowering drugs or statins on their own once they are secure in their bodies and their ability to heal, mistaking the drug’s limiting effect on their cholesterol levels for normal bodily function. And the cholesterol quickly returns to normal.

How frequently people quit statins after a heart attack was discovered by research published in JAMA Cardiology a few years ago, including approximately 60,000 individuals aged 66 and older. Nearly one in five persons who suffered a heart attack had stopped taking statins within two years of the event. And about 2 out of 5 people did not take the medication exactly as directed. They either took it less often or at a lesser dose.
To lessen their chance of experiencing another heart attack or stroke. These people have already experienced one must take statins or other cholesterol-lowering medications for the rest of their lives. Why, then, do statins work? They function by obstructing a component that your body requires to produce cholesterol. They also stabilize the plaques on blood vessel walls and minimize the risk of blood clots, in addition to decreasing cholesterol. Clotting is typically connected to the heart.
However, it can occur in any cardiovascular artery, resulting in brain strokes and the paralysis they cause. Blockages in the arteries that supply the kidneys and the limbs may cause renal issues or require amputation. Fresh blood cannot get through to supply organs and other tissues below the obstruction when the plaque blocks limb arteries. Peripheral Artery Disease (PAD) is a condition that primarily affects the toes and feet and can be so severe that patients lose their limbs.
Statins, which lower cholesterol, provide two preventative benefits. First, they are given for the main reasons for high-risk individuals who have poor blood indicators and are genetically prone to heart disease. The secondary cause is the commencement of the heart attack, which aids in preventing future recurrences.

Other than statins, there are new medications available to lower LDL cholesterol. These are injection-only PCSK9 inhibitors, such as Repatha. A 140 mg injection is administered subcutaneously twice a month to control LDL cholesterol. You must save up to Rs 30,000 because each injection costs Rs 15,000. Statins are more affordable. Ezetimibe is another medication that comes in tablet form. However, statins or Repatha are more effective.
Ask your cardiologist to adjust the dose, so you don’t have any adverse effects. Your body can adapt to the dosage if statins are producing side effects you can’t tolerate, such as digestive problems, muscular discomfort, or sleep problems. Some people do not require the exact dosage as previously since they feel better. But patients must remember that their ultimate objective isn’t taking less medicine but reducing their risks of experiencing another heart attack, bypass surgery, or stent.
Reasons why one should not stop taking statins:
In particular, statins can reduce LDL cholesterol (often known as “bad” cholesterol) by 30% to 50%, but if you stop taking them, these effects disappear.

Several people discontinue taking statins despite them having many advantages. However, it would help if you didn’t stop taking your statins unless you have a significant adverse effect or there is another severe medical cause (such as liver damage) for doing so. This is why:
- Heart disease and stroke are a result of high cholesterol.
- Statins increase lifespan and improve health. They also reduce mortality rates among those with excessive cholesterol.
- An increased risk of fatal cardiovascular events (such as heart attack or stroke) has been associated with stopping your statin.
- There are several statins available to try. If one doesn’t, there’s a good chance that another will. To explore if a different option is a better fit for you, work with your provider to transition from one to the other.
- Up to 75% of persons who stop taking a statin due to adverse effects can effectively rejoin it without experiencing any negative consequences.
- With time, statin-related side effects become bearable. Working with your healthcare practitioner, you might attempt a reduced dose or take your statin every other day as an alternative to quitting it altogether. This will usually eliminate any adverse effects you may have.
- Some adverse effects that patients encounter might not be brought on by the medicine or may originate from other sources (muscle pain is a good example).
- There are various generic choices for statins if the price is a concern. With the help of GoodRx, you may locate one that suits you at an affordable price.

Stopping Statins safely
Speaking with your healthcare practitioner is the only safe method to discontinue taking statins. The preventive advantages of statins often exceed the hazards for most people. However, there may be a few circumstances where doctors advise you to discontinue taking your statin.
Your doctor may suggest an alternate treatment for cholesterol, such as ezetimibe (Zetia) or a PCSK9 inhibitor drug, if trying a new statin drug or reducing the dosage of your current statin doesn’t work. Always discuss quitting a statin prescription with your doctor before doing so.