The outbreak of monkeypox is still a public health emergency, according to the Department of Health and Human Services (HHS).
The HHS first published the declaration on public health in August. According to the U.S. Centres for Disease Control and Prevention, over 28,000 instances of monkeypox have been identified in the country, and eight people have died as a result. As soon as the first case of monkeypox was discovered in the United States in May, the number of cases immediately increased, prompting demands for immunizations.
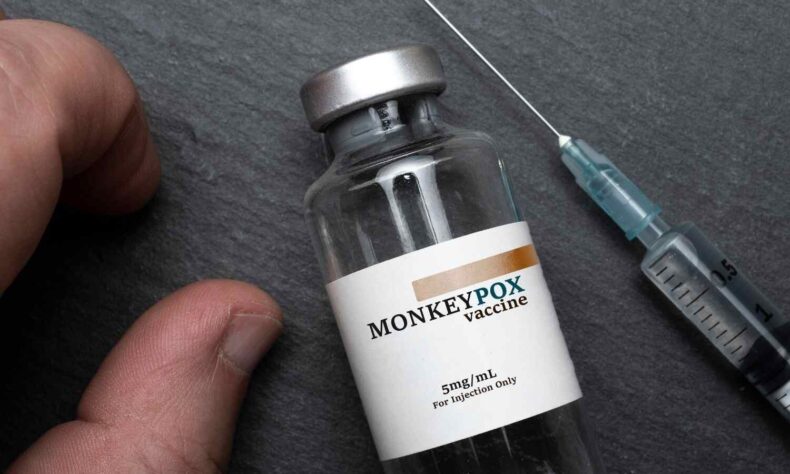
Over 1 million vaccinations have been given across the nation since they were launched in the summer. Their implementation, though, hasn’t been entirely simple.
What’s going on with the vaccinations for monkeypox?
Due to low-dose supplies, only a select few people were declared eligible for the shot, which sparked a rush for immunisation appointments. Because of this, the Food and Drug Administration (FDA) permitted the division of a single dosage into five to reach more individuals, raising fears that the amount of protection may be lowered.
A red, uncomfortable mark is appearing at the injection site for some patients in the meantime. This possibility, according to some publications, is preventing recipients—primarily males who have had sex with men—from receiving either their initial or follow-up dose, in part out of fear of stigmatisation.
How vaccinations against monkeypox are given
It’s critical to comprehend how most vaccinations are administered before diving into concerns about lower dosages, regardless of the condition they are intended to prevent. Injectable vaccinations come in three different forms: intradermal, subcutaneous, and intramuscular.
Dr Michael Chang, an infectious diseases expert at UTHealth Houston and Memorial Hermann Hospital, said that the majority of vaccines that are now available, such as the SARS-CoV-2 or influenza vaccines, are intramuscular injections.
Intramuscular injection sites in the upper arm or leg are prevalent. Furthermore, he added, “injecting deeper into the muscle enhances the immune response to the vaccination, maximising protection” for most authorised or completely approved vaccines. The incidence of local injection site responses is reduced as well.
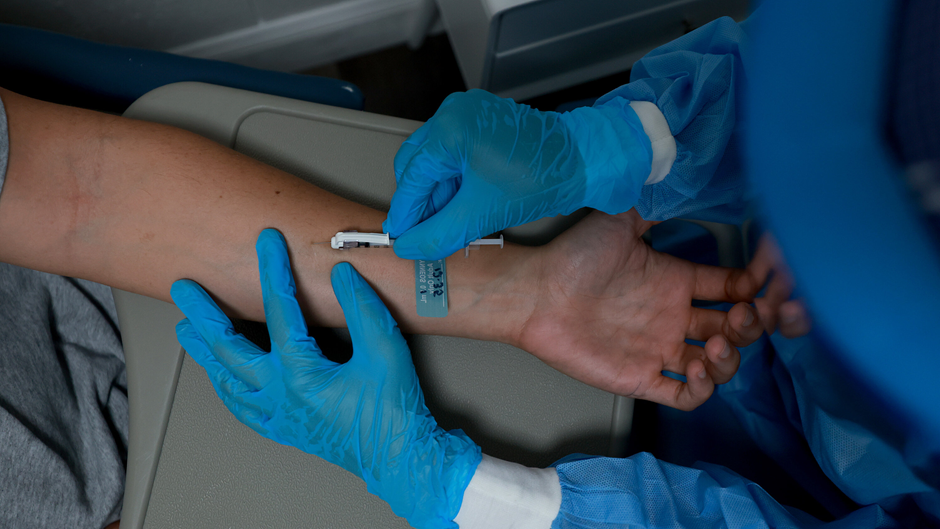
In subcutaneous injections, the needle is “inserted into a layer deeper than the skin, frequently the fatty layer between the skin and the muscle,” according to Chang. The JYNNEOS monkeypox vaccine was the first to be approved for distribution in this manner.
According to Chang, the method “isn’t used as frequently for vaccinations because you get more local site injection responses and the immune response in the skin may not be as robust.”
This brings us to the intradermal injection, which administers an immunisation to the epidermis of the skin. Vaccines for monkeypox are currently administered using this technique. Then why the change?
Dr Sujal Mandavia, chief medical officer of Carbon Health, said that intradermal vaccinations frequently need a lower dose to be effective.
This is because the delicate layers of our skin’s immune system prefer to respond quite strongly when exposed to foreign substances like vaccines.
Due to vaccination shortages, the intradermal method allows doses to be divided into fifths. David M. Souleles, MPH, director of the MPH Program and Practice at the University of California, Irvine, stated that “We can increase the overall supply now in place and immunise more at-risk individuals.”
However, Chang added that children under the age of 18 should still receive the immunisation subcutaneously instead of intradermally.
Will you get weaker protection due to the lower dose?
You might think that if you just get 20% of the usual monkeypox vaccination dosage, you won’t be immune against the illness, but according to the research, this is not the case.
According to Mandavia, the FDA decided to use a lower dose of immunisation and deliver it intradermally “based on this clinical research including 524 individuals.” “The study found that when one-fifth of the JYNNEOS vaccine is administered intradermally into the skin, it induces an immunological response comparable to a “full” dosage of subcutaneous injection.”
While the present immunisation provides protection, greater research into the degree of defence it provides over time is required. “The effect of the one-fifth intradermal dosage on long-term immunity and resistance to monkeypox is unknown at this time,” Chang noted.
When should you get a follow-up dose?
To get maximum benefits, you might think you’ll need four follow-up dosages, but fortunately, that’s not the case. Souleles explains that if you’re administered two doses of the monkeypox vaccine intradermally (28 days apart), then you’ll be completely immunised and protected.
If you are under the age of 18 and have your immunisation administered subcutaneously, your second dose should be administered 28 days after the first.
Peak immunity is predicted 14 days following the second JYNNEOS vaccination injection, Chang noted. But the problem is that data from the Centres for Disease Control (CDC) show that second-dose coverage is poor.
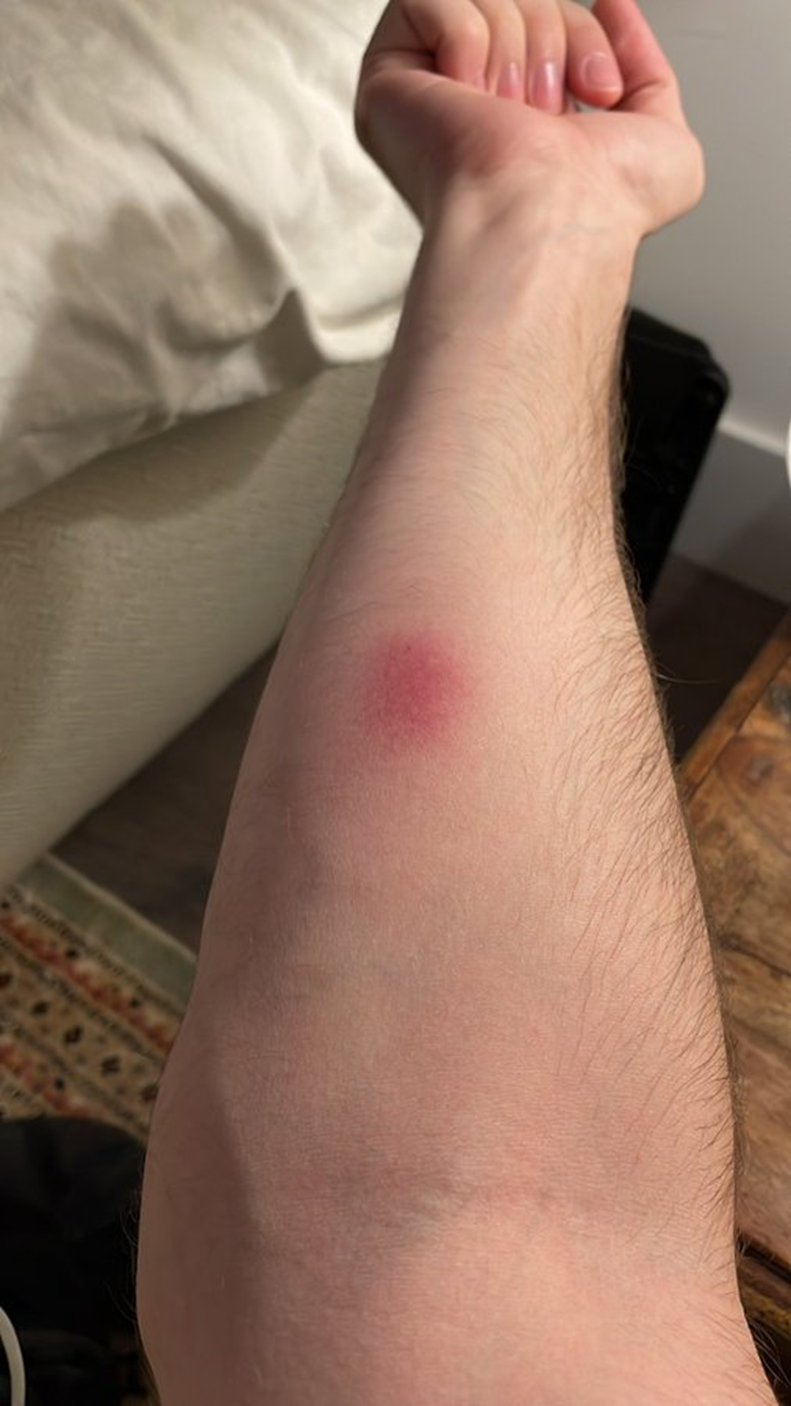
Why are people skipping the second dose?
One of the primary reasons people skip the second dose of the vaccine is that it leaves a red, sore mark at the injection site. It has been found that a reaction like this is not limited to the monkeypox vaccine, as Chang says that it is a common reaction to any intradermal injection and not just the JYNNEOS vaccine.
Mandavia says that the reason for it is that the immune system responds to it as a foreign substance and reacts against it.
Souleles says that reactions like this often result from COVID or flu vaccines and leave your arm or the site of the injection sore for a couple of days.
Mandavia assures that, though it might be uncomfortable to deal with, it is completely harmless.
For people who are concerned that another mark will appear after the second dose, they should request the injection at a less visible intradermal site like the shoulder or the upper back just over the shoulder blades, Chang explained.
New Monkeypox Testing Is Being Conducted
Testing for monkeypox before symptoms appear might be challenging. Patients typically wait until lesions have already emerged before contacting their doctor to get tested since early symptoms might be similar to those of other sexually transmitted diseases (STIs).
Benjamin Pinsky, MD, PhD, is the medical director of the clinical virology laboratory at Stanford Health Care, and his lab routinely receives requests to check bodily fluid samples for STIs including gonorrhoea and chlamydia.
When the lab performs an internal monkeypox test on samples from individuals without lesions, the monkeypox virus can occasionally be identified in these samples. Non-lesion samples have more false negative findings than lesion swabs do, according to Pinsky. However, it could be advantageous to screen for monkeypox cases in addition to other STIs.
Read also:https://tdznkwjt9mxt6p1p8657.cleaver.live/monkeypox-global-health-emergency-declaration/